We’ve all heard of knee and hip replacements, but have you heard of a total shoulder replacement?
If your doctor has spoken to you about the possibility of a shoulder replacement, you may have a lot of questions. We know a thing or two about shoulders.
Total shoulder replacements (or total shoulder arthroplasties) allow people with shoulder joint issues, like arthritis, to return to their normal lives with less pain.
As with any major joint replacement surgery, it has its limitations. You no longer have the same anatomical joint in your body. But when you’ve been living with unresolved pain for years, some post-op limitations are a welcomed trade-off.
If you haven’t already attempted conservative care for your pain and limitations, consider visiting JACO Rehab for a consultation. And if you need the joint replacement, we will see you in the clinic after your surgery!
The Shoulder Joint
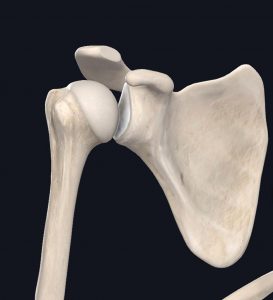
The shoulder joint is where your humerus and shoulder blade meet. The head of your humerus aligns with the glenoid of the shoulder blade to create a very mobile ball-in-socket joint. Your shoulder allows you to reach overhead, itch your back, wipe your bum, strap your bra, lift groceries, drive… it has such diverse functions because of its flexibility!
Images courtesy of Complete Anatomy
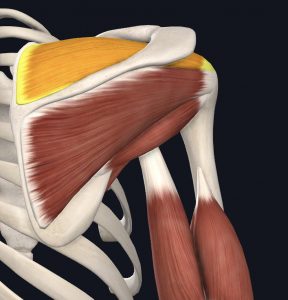
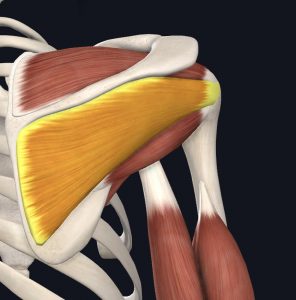
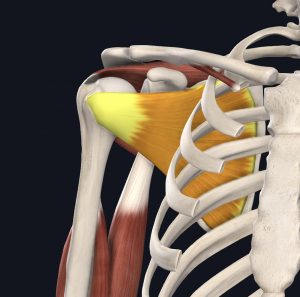
A flexible joints need excellent muscular and ligamentous support to maintain stability. Your rotator cuff, a group of small muscles around the shoulder, is crucial to the health and functionality of the joint. There are four muscles in the rotator cuff, each equally important to the integrity of the shoulder.
- Supraspinatus
- Infraspinatus
- Teres Minor
- Subscapularis
Images courtesy of Complete Anatomy
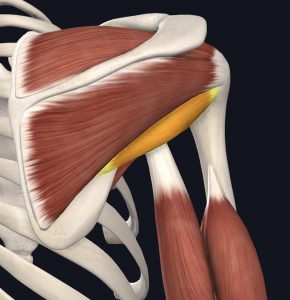
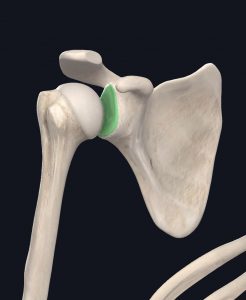
The shoulder joint also has cartilage to help create smooth movement. The cartilage sits in the glenoid and is called your labrum.
- Labrum (highlighted)
Images courtesy of Complete Anatomy
Issues in shoulder health arises when the labrum or the rotator cuff develop painful tears or degenerate over time. Some issues resolve themselves, but some persist.
Depending on the situation, surgical care is not always the first approach. If the tear is small or the pain is manageable, you may begin care with physical therapy in an effort to avoid unnecessary surgical intervention. You can read about non-surgical rotator cuff tear rehabilitation on our website.
When there are larger tears that cause more pain and dysfunction, surgery to address the tear may be warranted. You can also read about surgical approaches to rotator cuff tears on our website.
But when the shoulder’s structural integrity is damaged, whether it’s the joint or the surrounding tissues, a joint replacement could be the best option. This is especially true if conservative care has failed or major dysfunctions and pain limitations exist.
Types of Total Shoulder Replacement Surgeries
There are three types of shoulder replacements. Each one is appropriate for different conditions. They all have slightly different rehabilitation plans to honor the prosthetic’s integrity.
Anatomical Total Shoulder Arthroplasty (TSA) Surgery
An anatomical TSA is required when the joint is damaged, but the surrounding rotator cuff muscles are intact and healthy.
Examples of conditions where an anatomical TSA is needed include: (2)
- Arthritis (either degenerative or traumatic)
- Necrosis of the bone, which includes the glenoid
- Inflammatory joint conditions
In this case, the ball-in-socket joint is replaced with a similar ball-in-socket prosthesis.
Hemiarthroplasty
A hemiarthroplasty is required when the head of the humerus is damaged, but the rest of the joint is intact.
Examples of conditions where a hemiarthroplasty is needed include: (2)
- Necrosis of the humerus without glenoid involvement
- A humeral head fracture
Rather than replacing both the ball and the socket, only the ball becomes a prosthetic while the socket is untouched.
There are many cases where the surgeon may advise an anatomical TSA or reverse total shoulder replacement rather than a hemiarthroplasty despite your presentation, as there are certain situations where a full joint replacement may have better outcomes. (1)
Usually, this decision is made if the doctor is concerned with the future health of your glenoid (the socket). If they thinks that your glenoid may also need surgical attention in the future, they may advise to replace the whole joint at once.
Reverse Total Shoulder Replacement (rTSA) Surgery
A rTSA is required when the rotator cuff muscles aren’t salvageable, or in cases where the shoulder needs additional fixation or stabilization.
Examples of conditions where a rTSA is needed include: (2)
- Massive rotator cuff tears
- Severe inflammatory arthritis with massive cuff tears
- Failed anatomical TSA or hemiarthroplasty
- Humerus fractures that did not heal well
- Reconstruction after a tumor removal
In this case, the ball-in-socket joint is reversed. It becomes a socket-in-ball joint, which decreases the joint’s flexibility but improves its stability in the absence of stabilizing rotator cuff muscles (except the subscapularis, that usually stays).
You can still move your arm when it’s appropriate. Your deltoid takes over much of the work.
Even in its early stages, this surgery has been very successful in decreasing pain. The trade-off is loss in some function since it’s no longer as flexible and some musculature is lost. But, for many, this is a welcomed trade-off considering the long history of unresolved pain. (3)
Anatomical Total Shoulder Replacement Physical Therapy Protocol
Anatomical and reverse total shoulder replacements have their own treatment approaches. In this piece, we will discuss anatomical TSAs so we don’t confuse the two.
After your surgery, you will likely be in a sling for three to four weeks depending on your specific doctor’s recommendations. This is to protect the prosthesis as it begins to heal into the bone.
Movement precautions depend on the surgeon’s approach to cutting through the deltoid. However, most protocols advise to avoid…
- extending your arm (moving the arm behind you)
- placing weight through the arm
- excessive reaching/activity including driving
- lifting items
…until cleared to do so.
You can usually start driving safely after one month, and allowing the arm to extend behind you after six to eight weeks.
What Does Physical Therapy and Recovery Look Like?
Total shoulder replacement recovery has a general timeline, although it does differ person-to-person.
During the first six weeks of physical therapy, the main focus will be gaining range of motion and while protecting the prosthetic. Exercises will consist of gentle ranging of the joint, but no intense stretch. Your physical therapist will help you move the shoulder passively at first, then teach you how to stretch with assistance at home.
After six weeks, you will start to perform more active ranging and strengthening. The goal after 6 weeks is to progress your active movement towards lifting and reaching goals. If you have specific goals of your own that are specific (getting back to a sport or hobby), make sure you tell your physical therapist. You can discuss how to get there together.
Around six months post-op, you will graduate from physical therapy (yay!) with a home exercise program to make final improvements on your own.
In the long-term, you may have lifting precautions set by your surgeon. You will want to clarify these at later follow-up appointments.
Full recovery is seen at 1-2 years. It takes time to develop strength in the shoulder and return to your usual level of function. It can take a while for our shoulder to get back to a functional level, depending on how long it was injured before surgery.
At full recovery, you should be able to return to some sports like swimming and golf. Repetitive overhead exercises will likely be discouraged to preserve the joint and avoid future revisions.
Remember: Everyone’s recovery process looks different. Never get discouraged if your timeline differs from the one above. Recovery depends on the surgeon’s protocols, your anatomy, any complications, and daily life factors.
Physical therapists are here to help you problem-solve your particular situation. Are you a recovering caretaker? Are you trying to return to work? We do what we can to help you navigate your circumstances and recover as best you can.
The best thing you can do to ensure successful recovery is to be compliant. By understanding your physical therapist’s expectations and performing exercises as prescribed (just like taking medicine), you’ll increase likelihood of staying on-track with your rehabilitation.
Ask a Physical Therapist
At JACO Rehab, we rehabilitate shoulder injuries and surgeries all the time. Shoulder injuries are one of the most common conditions that walk into our clinics, and all therapists are fully qualified to treat any shoulder issue that presents itself.
Check out other pieces that discuss surgical and non-surgical rotator cuff injuries to learn more about the shoulder or share with a friend who may need some guidance.
If you would like to talk to a physical therapist prior to your surgery, call JACO Rehab and schedule a 10-minute consultation or a prehabilitation appointment to discuss expectations, ways you can prepare, and even things you can do prior to surgery to get a head start.
You don’t (and shouldn’t) have to go through total shoulder replacement recovery alone!
Written by Nicole Hernandez, DPT
Sources
1. Antuna SA, Sperling JW, Cofield RH. Shoulder hemiarthroplasty for acute fractures of the proximal humerus: a minimum five-year follow-up. J Shoulder Elbow Surg. 2008;17(2):202–9.
2. Sanchez-Sotelo J. Total shoulder arthroplasty. Open Orthop J. 2011 Mar 16;5:106-14. doi: 10.2174/1874325001105010106. PMID: 21584206; PMCID: PMC3093753.
3. Sirveaux F, Favard L, Oudet D, et al. Grammont inverted total shoulder arthroplasty in the treatment of glenohumeral osteoarthritis with massive rupture of the cuff. Results of a multicentre study of 80 shoulders. J Bone Joint Surg Br. 2004;86(3):388–95.