Did you recently suffer a rotator cuff tear? If your injury was severe enough, your doctor may have mentioned surgery for your shoulder. Rotator cuff surgery is very common, but they do require some work to rehabilitate. Luckily, physical therapists are here to help.
Keep reading to fully understand what rotator cuff surgery entails, including the healing timeline and recovery process.
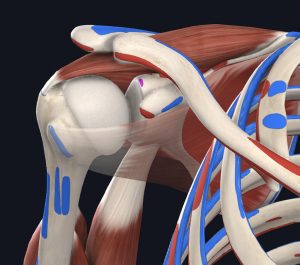
About Shoulder Anatomy and the Rotator Cuff Muscles
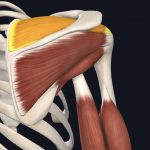
The rotator cuff (RTC) is a group of four muscles located on your scapula (shoulder blade), which attach to your humerus (upper arm bone). These muscles are responsible for holding your humerus in place, elevating your arm overhead, and rotating the shoulder.
These muscles can be remembered by the acronym “SITS”:
- Supraspinatus
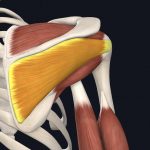
- Infraspinatus
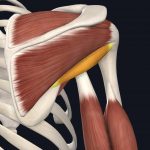
- Teres minor
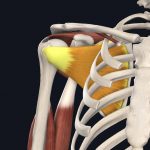
- Subscapularis
If any of these muscles are strained, torn, or inflamed, you could experience pain and weakness with an inability to lift your arm.
- Supraspinatus
- Infraspinatus
- Teres Minor
- Subscapularis
Images courtesy of Complete Anatomy
Pain can sometimes refer down the side of your arm or even into your hand which can be confused with nerve issues. This type of pain can develop from trigger points, inflamed muscles, or a tear.
The most common ways to injure your rotator cuff include:
- performing overhead tasks
- causing repetitive stress to your shoulder during throwing and racquet sports
- participating in contact sports with direct trauma
- experiencing wear-and-tear over time from poor shoulder girdle alignment and mobility
Your surgeon may opt for surgery over conservative care if you meet at least one the following:
- The tear is larger than three centimeter with good health of the surrounding tissue.
- The tear is “complete”, meaning the tendon has been completely pulled away from the bone.
- Your symptoms are chronic, meaning they have lasted six to twelve months.
- You have significant weakness and loss of use of your arm.
- Your tear was recently caused by a traumatic injury.
The most commonly repaired rotator cuff muscle is the supraspinatus, followed by the infraspinatus and subscapularis.
SLAP Tears Often Occur with a Rotator Cuff Tear
The glenoid labrum is a fibrocartilage disc in the shoulder joint which helps improve stability of the shoulder joint, but it can be injured with a rotator cuff tear.
One vulnerable spot is where the long head of the biceps tendon attaches along the cartilage in the shoulder. When that’s torn, it’s called a superior labral tear in the anterior to posterior direction—more commonly known as a SLAP tear.
- SLAP tear can occur here (dot in pink). This is also the attachment site of one of the biceps tendons.
Images courtesy of Complete Anatomy
SLAP tears can occur together with a complete rotator cuff tear because they both have common causes, including:
- motor vehicle accidents
- a fall onto an outstretched arm
- rapid pulling/forceful movement of the arm due to heavy weight or a sports-related injury
Those with any labral tear may experience a sensation of locking, popping, clicking, or grinding as well as a feeling that the shoulder may “pop out” along with loss of range of motion and weakness.
If you have both a complete rotator cuff tear and SLAP tear, you may experience a longer recovery time since there are more healing factors in your protocol.
What to Expect on your Surgery Day
Here’s what to expect as you prepare for your surgery day.
Inpatient vs. Outpatient Stays
Surgery can either be inpatient, where you stay in the hospital for several days, or outpatient, where you are able to return home the same day. The severity of the tear, your surgeon’s preference, and other factors related to your medical history may affect whether the surgery is inpatient or outpatient.
Incision Size
Most rotator cuff repair surgeries are performed arthroscopically and are outpatient procedures, as this is the most minimally invasive option. Your surgeon will make several small incisions surrounding your shoulder and insert a camera or arthroscope to be able to visualize the tissues needing to be repaired.
There are instances that the surgeon needs more visibility. Your surgeon may opt for a larger incision size if:
- Bone spurs need to be removed around the shoulder
- The tear is larger three to five centimeters
- A tendon transfer needs to be performed, the surgery may be mini-open or fully open.
Surgeries that require larger incisions are considered mini-open or fully open procedures. In a mini-open procedure, the surgery is performed partially by arthroscopy and partially by making a larger incision to allow the surgeon to physically visualize a larger area. With a fully open procedure, the surgeon makes a large incision to visualize the working area and performs the surgery without the use of arthroscopy.
Incision Aftercare
Steri-strips or other bandages will be placed over the incisions to decrease the risk of infection. Do not remove the steri-strips or bandages unless instructed by your surgeon. Most of the time, they will fall off on their own as the adhesive wears away.
Watch out for excessive bleeding, although some bleeding is normal and expected. Monitor incisions for signs of infection, like abnormal discharge (yellow, green, or pus-filled) or odor coming from the surgical wounds. Also monitor for any signs and symptoms of a deep venous thrombosis (DVT), including:
- Shortness of breath
- Difficulty breathing
- Extreme redness and warmth around the surgical area
If any of these arise, follow-up with your surgeon as soon as possible to avoid further complications.
Slings and Protection
In some instances, you will be instructed to wear a sling to protect the repaired tissue. Your surgeon will provide proper instructions regarding when and how long you must wear a sling to allow for proper healing. Sling-wear can range from a few days to a few weeks.
Rotator Cuff Repair Healing Timeline
Some good news! A rotator cuff repair surgery involving one tendon has an average success rate of 95%. A repair involving two tendons has an average success rate of >70%.
Depending upon the degree of the tear, healing times can range greatly:
- 4 months for a small tear
- 6 months for a large tear
- 6 to 12 months for a massive tear
Successful recovery requires a physical therapist’s guidance, but you’re in charge of following your precautions and staying consistent with your treatment plan.
Most patients start physical therapy a day or two after surgery. This largely depends upon your surgeon’s protocol and degree of tissue damage. There are cases where physical therapy starts after six weeks.
Be sure to discuss with your surgeon when you need to be starting your physical therapy at JACO Rehab so you can schedule your evaluation on time.
Rotator Cuff Repair Protocol
You need to be aware of the general protocol after the surgery. There are rules after surgery so that you do not re-injure yourself head back to the operating room.
Keep in mind that this is only a typical timeline and protocols can vary.
- Week 0-6: Start physical therapy. Passive range of motion ONLY. Do not move your arm! You could tear the muscle again while it’s still healing. There’s a major emphasis on protecting the surgery, reducing swelling, and restoring mobility in the shoulder during this time.
- Week 6-8: Begin active-assist range of motion as tolerated. This means moving the arm with assistance – but still not lifting it on your own. Your physical therapist will determine if you’re ready. Some protocols allow light strengthening if appropriate.
- Week 8-12: Active range of motion and strengthening begins. You can start contracting the rotator cuff muscles as tolerated, being careful not to overload the tendons as they adapt to added resistance. Again, your physical therapist will determine if you’re ready.
- Week 12+: Progressive strengthening and functional movements such as lifting, pushing, and pulling as tolerated.
Please understand that this is a rough timeline and does not always apply to each patient. It depends largely on what the surgery entailed, and some surgeons will make adjustments to this protocol if they see fit.
Each recovery story is unique, and each step is carefully progressed by your physical therapist to make sure you stay on the right path.
Remember that recovery is not a race. It takes time. Patience is key.
What to Expect at Physical Therapy
The first session will always consist of a thorough evaluation to assess your passive range of motion. only passive range of motion at this point to protect the healing tissues. Typically, you will be unable to actively lift your arm up, out to the side, or behind your back for about six to eight weeks. Your surgeon’s protocol will dictate your progression in physical therapy.
Things to keep in mind for your first session:
- Arrive early to fill out any necessary paperwork and have your ID and insurance card ready.
- Wear athlete clothing, and if comfortable, something sleeveless. Your physical therapist can assess the tissues and joints hands-on.
- Think about your goals. Which activities are you excited to return to after physical therapy?
Remember: We are here to help you not only by treating your injury directly, but by making you an integral part of your rehab team. This means that you should know how the exercises we are prescribing are addressing your issues.
Typical course of care for a rotator cuff repair will depend upon severity, location, and your own medical history. Expect to see a physical therapist for at least 12 weeks, two times per week.
Sessions typically include some hands-on manual therapy, which allows the therapist to address any tissue or joint mobility restrictions, which may be causing pain or underlying inflammation or irritation. As you improve, expect more exercises in your rehabilitation regimen. Come ready to work!
By taking measurements at the beginning and end of each session your physical therapist can ensure that the interventions prescribed are working for you and individualized to meet your goals such as getting back to work, surf, or golf!
Exercises for Surgical Rotator Cuff Tears
Here are two examples of home exercises that a physical therapist may prescribe directly after a rotator cuff repair. You can ask your surgeon what exercises you can start doing before you see physical therapy.
Be careful trying exercises on your own, as they may break protocol. These are typically within protocol if you do them correctly.
Check with your surgeon before you try these, or wait for your first physical therapy session.
1. Shoulder external rotation stretch at a table or with a dowel: You want to keep these motions as passive as possible. Be sure to keep your chest up, squeeze your shoulder blades together, and keep your elbows tucked into your side to isolate the right movement. The goal is to stretch up to the point of pain but not past it during the early phases of rehab. Stretching past pain causes inflammation. It’s key to keep inflammation down to allow for natural healing to occur.
2. Table flexion stretch: This passive stretch emphasizes the range of motion needed to get back to activities overhead. All you need is a table or counter about waist height. Goal is to keep your shoulder down and back and neck relaxed while taking a step back to stretch your arms overhead. Again, avoid pain or pinching to keep inflammation minimal. You should be moving your body on your arm, NOT your arm on your body.
Reach out!
We wish you the best of luck with your recovery. To schedule an appointment with use please call (808) 381-8947 or visit our website for more information about our therapists and locations!
Written by Jenn Lewis, DPT.