Have you ever struggled with incontinence? Pelvic pain? Discomfort during sex? Inability to tolerate a medical pelvic exam? Your pelvic floor, or the muscular sling that sits under your abdomen, might be the culprit.
The pelvic floor has a significant impact on your daily activities. Just like other muscle groups in the body, the pelvic floor coordinates its contractions to help you do your everyday tasks, including lifting and running. But people don’t discuss pelvic floor health enough, maybe due to the personal nature of pelvic floor problems, cultural taboos, or general unfamiliarity with the muscle group.
Pelvic floor dysfunction, or the incoordination of the muscles in the group, is common and treatable. And yet, It is estimated that one in four women under the age of 80 will experience pelvic floor dysfunction, with that rate climbing even higher after 80 years of age (4). Those rates are rising too quickly—It’s time to discuss the pelvic floor.
It’s important to note that this is not only a women’s issue. Men can experience pelvic floor dysfunction too, which can include challenges like trouble urinating, incontinence following a prostatectomy, erectile dysfunction, or constipation (1).
So, what exactly is the pelvic floor? And is there anything that can be done about pelvic floor dysfunction?
Pelvic Floor Anatomy
The pelvic floor is a muscle group in the bottom portion of the pelvis, otherwise known as the pelvic outlet. This muscle group consists of a few layers that primarily function to support your pelvic organs, maintain continence, and contribute to healthy core function (2). Your pelvic floor actually is part of your core!
The pelvic floor muscles support the pelvic organs similarly to a hammock or sling along with other ligaments and structures inside of the body. They keep the bowels, bladder, and uterus in the correct position. Proper pelvic floor activation can also help you hold things in—a strong, coordinated pelvic floor can keep the end of the urethra (for urine) and end of the rectum (for feces) closed when it is needed, which prevents leakage.
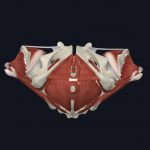
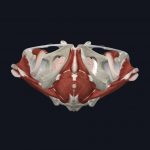
The pelvic floor muscle group is present in both male and female anatomy. The structures are different depending on a person’s sex due to differences in pelvic anatomy and function. For example, the female pelvis is wider than the male’s pelvis, so the pelvic floor spans over more space.
- Female pelvic floor (from below)
- Male pelvic floor (from below)
Images courtesy of Complete Anatomy
Why is the Pelvic Floor Important?
A healthy pelvic floor is important for activities such as:
- Core exercises: The pelvic floor is one of your core muscles, and therefore a very important part of effective core activation.
- Lifting: Proper pelvic floor activation and abdominal pressure control reduce risk of back pain, especially for pregnant and postpartum populations (3)
- Intimacy: Pelvic floor dysfunction may lead to sex being painful or challenging,
- Voiding: An underactive pelvic floor can make it difficult to maintain continence, and an overactive pelvic floor may make it challenging to void (pee and poop).
When functioning well, the pelvic floor is able to adapt to the stresses we put on the body to maintain continence and support of the pelvic organs. When the pelvic floor is not functioning properly, you may experience leakage, pain in the pelvic region, difficulty urinating, constipation, pain with sex, inability to have sex, inability to get routine pelvic exams, prolapse, or combinations of these things.
Things that may affect pelvic floor function include:
- Pelvic surgeries: These can create scar tissue, which can limit mobility of surrounding tissues and can feel uncomfortable.
- Pinched nerves or nerve damage: Common after giving birth or with lower back conditions, this may cause changes in muscle activation patterns.
- Pregnancy: You may experience increased strain on pelvic floor structures due to anatomical changes while carrying a baby to term.
- High impact athletics: Heavy plyometric activities can cause increased muscle tone, or an overactive pelvic floor, due to high physiological stress.
- Poor posture and breathing mechanics: This can put increased strain on the pelvic floor due to the increased pressure directed to the abdominal cavity.
If you are having symptoms that may be related to pelvic floor function, please talk to your gynecologist or urologist. They will be able to screen for underlying conditions and give you a referral to physical therapy if it’s right for you!
What is Pelvic Floor Physical Therapy?
Pelvic floor treatment is a specialty of physical therapy that focuses on pelvic floor muscle training, habit modification, education, relaxation, breathing exercises, and incorporation of those techniques into your everyday activities like squatting and lifting.
Pelvic floor physical therapy is much more than just “doing kegels.” In fact, if you have an overactive pelvic floor, kegels can be the opposite of what will help you! Your physical therapist will determine what you need and design a treatment plan based upon your evaluation.
What to expect during physical therapy
The session will start with an initial evaluation in which you and a physical therapist will discuss your symptoms, do some testing of strength, mobility, and function. Your therapist will explain what they are doing during your session and please feel free to speak up if you aren’t feeling comfortable. They will then get you set up with your home exercise program based on the findings during the evaluation.
It is important to do your home exercise program in order to get the full benefit from your sessions. You will review the home program and discuss any changes in symptoms at your next visit. Or, there may not be any change by the second visit—and that’s okay! It takes time to see changes during any rehabilitation effort.
As you progress, your therapist will incorporate more challenging activities similar to activities in your daily life to help improve function and progress you toward your goals.
When receiving physical therapy for your pelvic floor, communication is key in order to maintain a positive environment. Your pelvic floor therapist wants you to feel comfortable throughout the session. Please let your therapist know if you feel any discomfort or have concerns regarding symptoms or treatment.
Remember: As the patient, you have autonomy over your own body. You can always ask for more information on treatment and examination techniques.
If you’re feeling symptoms discussed in this article, tell your doctor to refer you to a pelvic floor physical therapist.
Written by Cira Pihl, PTA
Sources
1. Berghmans B, Nieman F, Leue C, Weemhoff M, Breukink S, van Koeveringe G. Prevalence and triage of first contact pelvic floor dysfunction complaints in male patients referred to a Pelvic Care Centre. Neurourol Urodyn. 2016 Apr;35(4):487-91. doi: 10.1002/nau.22733. Epub 2015 Jan 25. PMID: 25620671.
2. Cho ST, Kim KH. Pelvic floor muscle exercise and training for coping with urinary incontinence. J Exerc Rehabil. 2021 Dec 27;17(6):379-387. doi: 10.12965/jer.2142666.333. PMID: 35036386; PMCID: PMC8743604.
3. Kazeminia M, Rajati F, Rajati M. The effect of pelvic floor muscle-strengthening exercises on low back pain: a systematic review and meta-analysis on randomized clinical trials. Neurol Sci. 2023 Mar;44(3):859-872. doi: 10.1007/s10072-022-06430-z. Epub 2022 Oct 7. PMID: 36205811.
4. Kenne, K.A., Wendt, L. & Brooks Jackson, J. Prevalence of pelvic floor disorders in adult women being seen in a primary care setting and associated risk factors. Sci Rep 12, 9878 (2022). https://doi.org/10.1038/s41598-022-13501-w